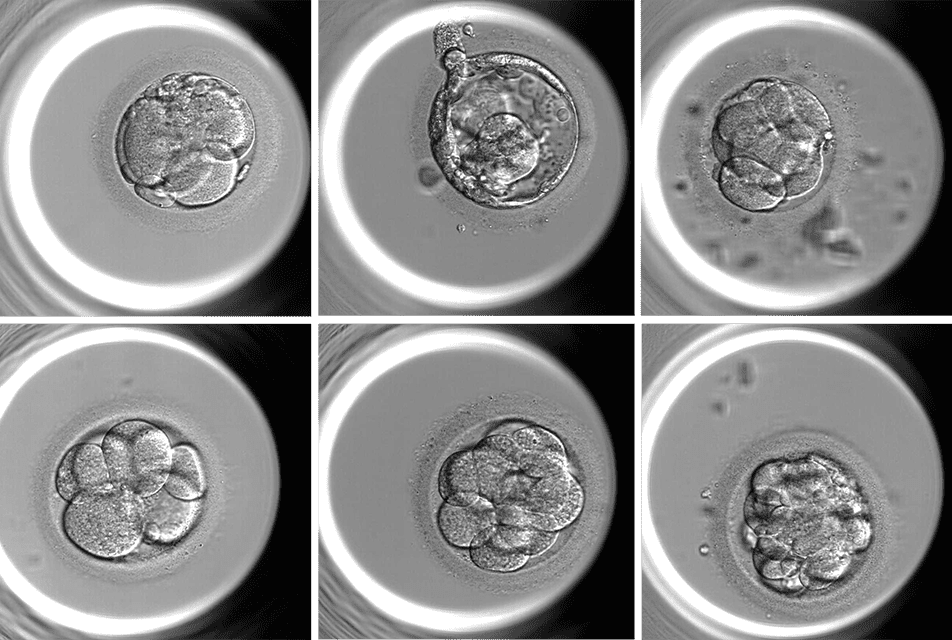
Researchers at Weill Cornell Medicine have developed an artificial intelligence-based system called BELA that can accurately assess the chromosomal status of in vitro-fertilized (IVF) embryos using only time-lapse video images of the embryos and maternal age. This new system is fully automated, objective, and does not require embryologists’ subjective assessments of embryos.
According to Dr. Iman Hajirasouliha, associate professor of physiology and biophysics, BELA offers a more accurate approach compared to prior methods, with greater predictive power due to the larger amount of image data used. The system was trained on a dataset of nearly 2,000 embryos and their ploidy status, and tested on new datasets from Weill Cornell Medicine and separate IVF clinics in Florida and Spain.
Dr. Nikica Zaninovic, associate professor of embryology, led the embryology work for the study, which also involved Dr. Zev Rosenwaks, director of the Center for Reproductive Medicine at Weill Cornell Medicine. If confirmed in clinical trials, BELA could improve the efficiency of the IVF process and expand access to IVF care globally.
Assessing IVF Embryo Quality with Artificial Intelligence
The success of In Vitro Fertilization (IVF) largely depends on the quality of the embryos used in the process. Currently, embryologists assess embryo quality by examining them under a microscope, which can be subjective and may not always accurately predict the chromosomal status of the embryo. To address this limitation, researchers at Weill Cornell Medicine have developed an artificial intelligence-based system called “BELA” that can accurately assess the chromosomal status of IVF embryos using only time-lapse video images of the embryos and maternal age.
Objective Assessment of Embryo Quality
Unlike prior AI-based approaches, BELA does not require embryologists’ subjective assessments of embryos. This makes it an objective and generalizable measure of embryo quality. The system uses a machine-learning model that analyzes nine time-lapse video images of an embryo under a microscope in a key interval about five days after fertilization to generate an embryo quality score. This score, combined with maternal age, is then used to predict euploidy (normal number of chromosomes) or aneuploidy (abnormal number of chromosomes).
The researchers trained the model on a deidentified dataset with image sequences of nearly 2,000 embryos and their PGT-A-tested ploidy status. They then tested the model on new datasets from Weill Cornell Medicine CRM and separate IVF clinics in Florida and Spain. The results showed that BELA predicted ploidy status with moderately higher accuracy than previous versions and worked well for both internal and external datasets.
Improving IVF Efficiency and Equity
The development of BELA has significant implications for improving the efficiency of the IVF process. By providing an objective and accurate assessment of embryo quality, BELA can help embryologists select the best embryos for transfer, reducing the risk of failed implantation or miscarriage. Additionally, BELA’s ability to process a vast amount of image data for each embryo suggests that it could be used for more than ploidy prediction, such as general embryo quality estimation and prediction of the embryo development stage.
Moreover, BELA has the potential to expand access to IVF care across the world, particularly in areas with limited access to high-end IVF technology and PGT testing. This could improve equity in IVF care globally, making it more accessible to a wider range of people.
Future Directions
The next step for the researchers is to test BELA’s predictive power prospectively in a randomized, controlled clinical trial, which they are currently planning. If successful, BELA could become a valuable tool in IVF clinics worldwide, improving outcomes and reducing costs. The researchers also hope to explore other potential applications of BELA, such as its use in predicting the risk of miscarriage or birth defects.
Overall, the development of BELA represents a significant advancement in the field of reproductive medicine, with far-reaching implications for improving the success rates and accessibility of IVF care.
External Link: Click Here For More